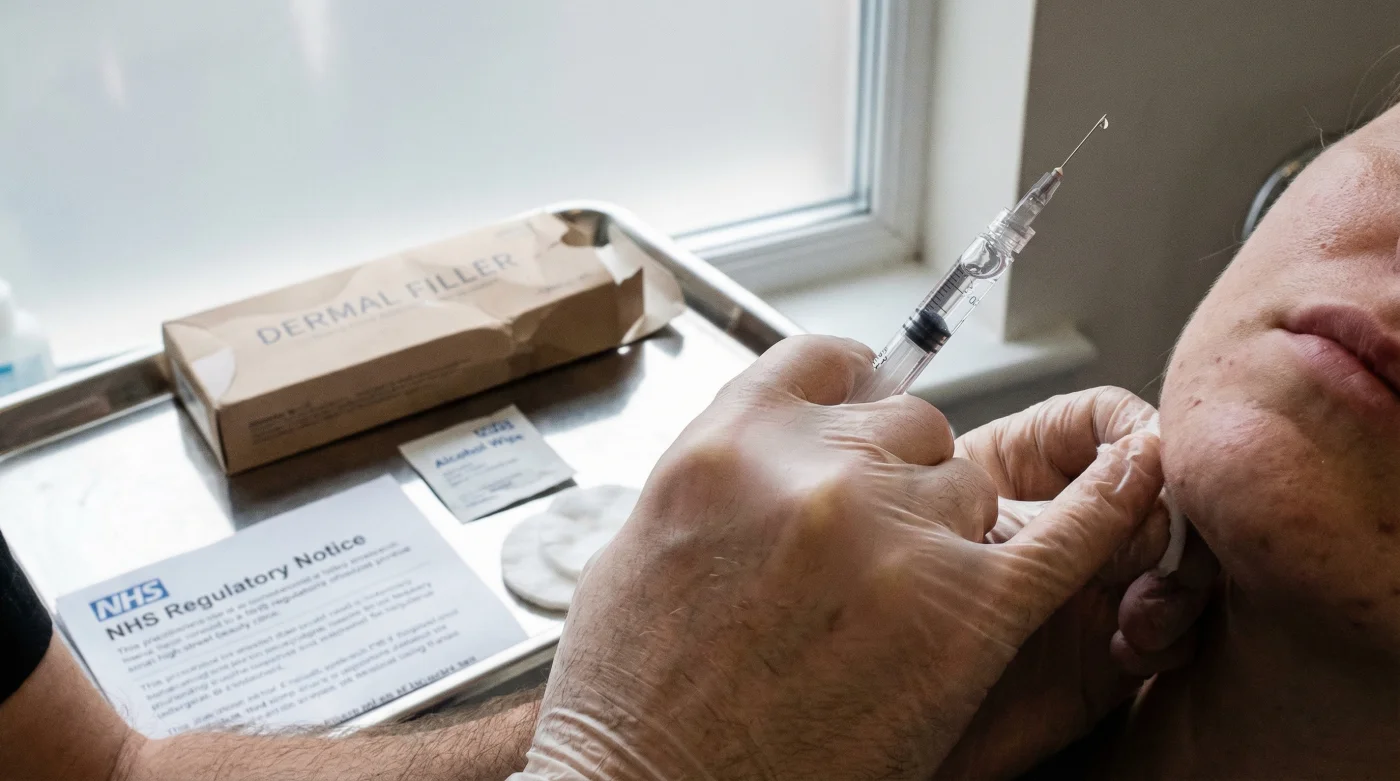
For years, popping down the local high street for a quick ‘tweakment’ has been as routine for many Britons as booking a haircut or picking up the weekly shop. However, behind the glossy salon facades and perfectly curated social media feeds lies a hidden, largely unregulated danger that has left thousands with permanent scarring, vascular complications, and severe psychological distress. The days of trusting your face to a weekend-certified injector are officially coming to an abrupt end, thanks to an impending and severe regulatory storm.
In a watershed moment for aesthetic medicine, NHS England alongside the Department of Health and Social Care confirms strict new licensing rules for high street dermal fillers, effectively triggering an immediate crackdown on local beauty salons. Before you even consider sitting in an injector’s chair this season, you must understand the one critical medical qualification that will soon separate the legal, safe practitioners from the outlawed operators who risk leaving you disfigured.
The Dawn of the High Street Crackdown
The UK has long been considered the ‘Wild West’ of the aesthetics industry, uniquely lacking the stringent legislative guardrails seen across Europe and North America. Until now, legally, a practitioner required zero medical training to purchase and inject complex dermal fillers. This loophole has fuelled an exponential rise in catastrophic aesthetic outcomes, placing an immense, avoidable burden on regional healthcare trusts and specialist plastic surgery units.
Clinical studies demonstrate that the rising tide of unregulated treatments correlates directly with a staggering increase in emergency corrective procedures. Experts advise that the impending legislation will implement a rigorous, two-tiered licensing system. This robust framework targets both the premises where treatments are performed and the specific competencies of the practitioner, ensuring that high street beauty salons can no longer operate as rogue, unchecked medical clinics.
| Practitioner Status | Patient Safety Level | Recourse in Emergency | Long-Term Results |
|---|---|---|---|
| Regulated Medical Professional | High (Strict infection control protocols) | Immediate prescription of reversal agents | Predictable, anatomically sound |
| Unregulated Salon Worker | Low (Basic hygiene only, non-clinical environment) | Total reliance on overloaded A&E departments | High risk of migration, asymmetry, and lumpiness |
To fully grasp why these uncompromising regulations are non-negotiable, we must look beyond the surface and examine the critical biological mechanisms at play during a seemingly simple injection.
The Clinical Reality Under the Skin
Dermal fillers are not mere cosmetic paints; they are complex, highly viscous medical devices implanted deep into the delicate facial anatomy. When an unqualified individual wields a syringe, they are navigating a treacherous minefield of major arteries, delicate veins, and vital nerves without an anatomical map. The inadvertent injection of just 0.1ml of dense filler into the wrong facial plane can instantly compromise blood flow, leading to irreversible tissue death within a matter of hours.
Diagnostic Guide: Recognising Critical Complications
- NHS England confirms strict new licensing rules for high street dermal fillers
- L’Oreal sets a new standard by eliminating synthetic microplastics from all scrubs
- Boots UK removes popular chemical exfoliants from shelves over new safety rules
- Vitamin C serums require a strict five minute wait before sunscreen application
- Fermented rice water rinses directly triple hair elasticity within three wash cycles
- Symptom: Severe, disproportionate pain accompanied by sudden skin blanching (turning white or mottled). = Cause: Vascular occlusion (filler directly blocking a major facial artery, starving tissue of oxygen).
- Symptom: Delayed-onset hard nodules appearing weeks or months after treatment. = Cause: Biofilm formation (a deep-seated bacterial infection requiring extended, targeted antibiotic therapy).
- Symptom: Rapid, asymmetrical swelling and intense heat 48 hours post-injection. = Cause: Localised erythema and severe oedema indicative of acute immune rejection or aggressive infection.
The chemical makeup of the filler itself drastically alters both the desired aesthetic outcome and the inherent risk profile.
| Filler Classification | Primary Component | Typical Dosing & Longevity | Clinical Reversibility |
|---|---|---|---|
| Standard Temporary Filler | Hyaluronic acid (HA) | 0.5ml – 2.0ml (Lasts 6-12 months) | Fully reversible with targeted Hyaluronidase |
| Biostimulator | Calcium hydroxylapatite (CaHA) | 1.5ml per session (Lasts 12-18 months) | Non-reversible, requires surgical extraction if severely compromised |
| Collagen Inducer | Poly-L-lactic acid (PLLA) | Varies by dilution (Lasts up to 24 months) | Non-reversible, must degrade naturally over time within the tissue |
Understanding the chemistry is only half the battle; knowing precisely who is legally permitted to hold the syringe is where the new law forcefully steps in.
The Mandated Medical Qualifications
Under the confirmed framework supported by NHS England, the days of a simple online or weekend certificate serving as a legitimate licence to inject are over. High street salons will soon face strict local authority enforcement, requiring practitioners to hold recognised, verifiable medical credentials before ever piercing the skin barrier.
The cornerstone of this new era is the Level 7 Diploma in Clinical Aesthetic Injectable Therapies. This postgraduate-level qualification demands extensive anatomical study, hundreds of hours of supervised clinical practice, and a profound, tested understanding of complication management. Furthermore, the administration of prescription-only emergency reversal agents dictates that clinics must either employ an independent prescriber or have one immediately on-site. If a practitioner cannot prescribe antibiotics or administer reversal enzymes within exactly 60 minutes of a suspected vascular occlusion, they will be operating entirely outside the law.
Key Operational Changes for Clinics
- Premises Licensing: Salons must pass rigorous local council hygiene and infection control audits, demanding standards akin to minor surgical units, including clinical waste disposal and sterilisation protocols.
- Age Verification: Strict, uncompromising enforcement of the Botulinum Toxin and Cosmetic Fillers (Children) Act 2021, mandating rigorous ID checks to protect vulnerable under-18s from predatory aesthetic marketing.
- Insurance Mandates: Comprehensive medical indemnity insurance will become a strict legal requirement, a safety net which unregulated practitioners will find fundamentally impossible to secure from reputable brokers.
With these stringent, industry-altering rules rapidly approaching, patients must urgently learn how to protect themselves in a shifting aesthetic marketplace.
Navigating the New Aesthetic Landscape
As the transition period begins, thousands of soon-to-be-unqualified high street injectors will undoubtedly attempt to mask their lack of mandatory credentials, offering heavily discounted treatments to clear their stock of unregulated, unverified fillers. This ‘grey market’ poses the greatest immediate threat to public health. Consumers must transition into becoming proactive auditors of their own healthcare, outright refusing to prioritise a bargain over fundamental biological safety.
Experts advise that you should always demand a comprehensive, obligation-free pre-treatment consultation. This must be a distinct, separate appointment occurring at least 24 hours prior to any injections, allowing for a legally mandated ‘cooling-off’ period. If a high street practitioner attempts to rush you from a brief chat directly to the injection chair in under 15 minutes, you must immediately walk away and report the premises.
| Assessment Criteria | The Green Flags (What to Look For) | The Red Flags (What to Avoid) |
|---|---|---|
| Practitioner Registration | Active, verifiable registration with the NMC, GMC, or GDC. | Only possesses generic ‘CPD’ certificates or weekend beauty course diplomas. |
| Product Transparency | Opens sealed boxes directly in front of you; freely provides batch numbers and expiry dates. | Pre-filled syringes drawn out of sight in a back room; unbranded or foreign-labelled vials. |
| Emergency Preparedness | Maintains an emergency kit on-site, with temperature-sensitive drugs stored correctly at 2°C – 8°C. | Cannot confidently explain their exact, step-by-step protocol for reversing a vascular occlusion. |
As these monumental regulatory shifts take hold, the UK aesthetic sector is finally maturing into a heavily guarded, recognised branch of medical practice, permanently altering the high street landscape for the better.
Read More